Ostomy
I sit in the urology office, surrounded by older men and pictures of penises. The door opens, and another man walks up to the desk. Some men are accompanied by their wives, but I am the only female patient. Having cancer can be very lonely; being a woman with bladder cancer is even lonelier.
 According to the American Cancer Society, in the United States, more than 81,000 people will be diagnosed with bladder cancer in 2022. Of those, 61,700 will be men, and 19,480, or 24%, will be women. Unfortunately, because the signs of bladder cancer, like blood in the urine, mimic gynecologic illnesses, they are written off as less serious. This attitude leads to lower survival rates for women, In fact, both the bladder cancer rates and the death rate from bladder cancer for women are expected to rise this year.
According to the American Cancer Society, in the United States, more than 81,000 people will be diagnosed with bladder cancer in 2022. Of those, 61,700 will be men, and 19,480, or 24%, will be women. Unfortunately, because the signs of bladder cancer, like blood in the urine, mimic gynecologic illnesses, they are written off as less serious. This attitude leads to lower survival rates for women, In fact, both the bladder cancer rates and the death rate from bladder cancer for women are expected to rise this year.
Like others, my cancer was attributed to other factors: fibroids, urinary tract infections, kidney stones, and old reliable, menopause. My cancer was found accidentally by my gynecologist during an ultrasound for the fibroids. I was lucky. Because of the delay, my cancer was large and appeared to have spread. After several scans and three surgeries to obtain tissue for pathology, I was lucky to only have Stage 1 bladder cancer. It had not spread but it was high grade. My cancer was aggressive and I had some decisions to make.
Bladder cancer is typically treated with BCG, or Bacillus Calmette-Guerin, a germ related to the one that causes tuberculosis. This is a type of immunotherapy. They insert the BCG right into the bladder using a catheter. It is held in for a couple of hours then voided out. This is performed in the urologist’s office once a week for six weeks. Unfortunately, there has been a BCG shortage for several years. Chemotherapy might be used instead. I went through a six-week cycle of BCG treatment then received a cystoscopy to see the results. Unfortunately for me, the cancer had grown back in several places, so we decided I would require a radical cystectomy. A cystectomy is a surgery to remove the bladder, lymph nodes, sometimes the urethra. In women, surgeons also frequently remove the uterus, fallopian tubes, ovaries, cervix, and sometimes a part of the vaginal wall (Basically, a hysterectomy). An alternate passageway for urine to pass is also built. These include a neobladder, Indiana Pouch, and an ileal conduit. A neobladder is considered a continent diversion in that an internal pouch is made out of intestine and attached to the urethra. With a neobladder, a person is able to retrain their bodies to void like they used to, albeit using different muscles.
An Indiana Pouch, or a continent cutaneous pouch, is also internal but must be emptied with a catheter through a stoma. No outside collection bag is required. The third type, an ileal conduit, is considered incontinent as there is no bodily control over voiding of urine. A piece of the ileum is attached to the ureters at one end and through an opening outside the abdomen, or a stoma, where urine flows into a collection bag.
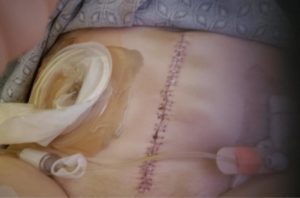 I received my ileal conduit, or urostomy, three years ago. It went by in a blur but there are some things I remember clearly, and some things I wished I had known. A radical cystectomy is major, life-changing surgery. My body is forever changed. I wear a urine collection device that is a daily reminder of my cancer. I deal with leaks and skin issues. I was able to take a class with ostomy nurses before my surgery. I was gaining an understanding of what to expect. I received help with changing my bag and had access to a visiting ostomy nurse. I continue to receive support from ostomy nurses at the hospital clinic should I ever need them (and I did for about a year).
I received my ileal conduit, or urostomy, three years ago. It went by in a blur but there are some things I remember clearly, and some things I wished I had known. A radical cystectomy is major, life-changing surgery. My body is forever changed. I wear a urine collection device that is a daily reminder of my cancer. I deal with leaks and skin issues. I was able to take a class with ostomy nurses before my surgery. I was gaining an understanding of what to expect. I received help with changing my bag and had access to a visiting ostomy nurse. I continue to receive support from ostomy nurses at the hospital clinic should I ever need them (and I did for about a year).
What I was unprepared for was the hysterectomy. I know I was not really informed about the effects of hysterectomy surgery. For example, I did not know about vaginal discharge after surgery. I often see that question asked on online forums. This surgery affects sexual function. Women often experience dryness or pain after and decreased desire. It can definitely have an impact on desire. It is important to discuss organ and nerve-sparing options with your surgeon. In the past, they just removed everything. Recent advances have allowed for more judicious surgery. Ovaries and vaginal walls may be spared, if safe to do so. If your surgeon doesn’t bring these issues up, please ask. It can be hard to know what questions to ask because we don’t know what we don’t know. I am always asking questions. I am glad I did. (I don’t know if my kids are because they were in the room with me when I asked my questions.)
There is so much information to process when you are looking at surgery. Your number one priority is saving your life. You are not always looking beyond the immediate future. Don’t forget what is important to you. You might need to fight for it. Like me, you may be the only woman in the office, but that’s ok. You got this!
