Ostomy

By the time I was diagnosed with bladder cancer in August 2016, I had been experiencing increasing pain, discomfort, and symptoms involving my urinary system for over two years. I had never heard of bladder cancer, so that diagnosis was not even on my radar. I didn’t know what was happening with my body; I just knew that something was not right, and because I was young and didn’t tick any of the boxes for being at risk for anything significant, medical professionals ignored my pleas for help all that time.
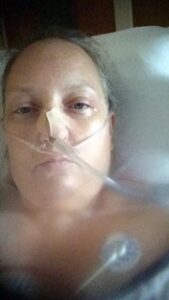 In mid-July 2016, I was so miserable, uncomfortable, and thoroughly exhausted since I was sleep-deprived from having to go to the bathroom urgently as often as every 5 minutes, even throughout the night, that I drove myself to the emergency room at a local hospital in the dead of night – in tears and doubled over in pain.
In mid-July 2016, I was so miserable, uncomfortable, and thoroughly exhausted since I was sleep-deprived from having to go to the bathroom urgently as often as every 5 minutes, even throughout the night, that I drove myself to the emergency room at a local hospital in the dead of night – in tears and doubled over in pain.
Some tests were run, and the attending doctor actually had the audacity to insinuate that the problems I was having were caused by my menstrual cycle. At nearly 41 years of age, I was highly offended by this. I assured him with expletives that I knew what hole the blood clots I was urinating came out of and that if he were urinating blood clots, he could tell because of how uncomfortable and painful the experience was. Laughing, he said, “I guess you’re right,” before telling me he would check on more results. Though he said he’d be back, I never saw the man again.
After a while, a PA was dispatched to my exam area to discharge me home with medications and no referral again.
I burst into tears.
Not just any tears, but the type of cry that would make anyone uncomfortable. A cry with tears as big as the Amazon and the Nile combined.
My breaking point had been reached.
After the PA verbally noted that my reaction was abnormal, I went on a tirade about how the responsibility of a diagnosis or a proper referral was ON THEM! They were the medical professionals, and as the patient, it was not my responsibility to figure out what was wrong with me. When I revealed that I’d been on the medications and in that ER before, she went digging in my electronic chart. A few minutes later, she returned with new discharge instructions, the prescriptions, and a ranked referral list.
I cried even more just from the sheer relief of finally being heard and receiving a referral.
The PA pointed at the referrals on the paper. “Start at the top of the list and work your way down. I ranked them according to who I would want to see if it were me. Go with whoever can get you in first.”
It was from that point that my medical world started snowballing. I got to see a urologist the next day. A week and a half later, I had a cystoscopy – if you don’t know what that is, think colonoscopy, except it’s for the other hole!
It took a couple of weeks to get in with my urology oncology surgeon, but when I did, it was extremely clear that saving my bladder was NOT an option. Even from the imaging, they could tell that the primary tumor had grown through my bladder wall. I was going to need a diversion.
At the time, I was an administrative assistant in a pediatric GI office. One of my nurse friends, Jeanne, was with me for the appointment. I knew what ostomies were already. I had not seen them in person, but I knew I could have a long, good quality of life with them.
My physician gave me my surgical options—ileal conduit with a urostomy OR a neobladder.
Neo-what?! I had yet to learn what that was and asked for the weekend to do the research on my own.
I discussed everything with Jeanne as she drove me home, then did a lot of Googling before discussing the options more with my GI friends, including Dr. Sam, one of the physicians I supported.
When I called Dr. Sam, I already had facts and just needed to talk through the options with someone. I told him the options I was given and that I was not feeling very encouraged by the data I read with the neobladders. He asked me some questions regarding data and how I felt about things. Then he assured me that he personally would make the same decision I was naturally leaning towards – the urostomy.
Honestly, I was at least tenfold more upset about needing to endure chemotherapy than I was an 8-hour surgery to have my bladder removed and an ostomy placed. I continued to move forward with treatment over eight months.

Liz raising awareness about the importance of ostomies.
I had a lot of ups and downs, but choosing my urostomy was the most straightforward decision I had to make during that time. I am now seven years out, and it was one of the best decisions ever.
Both my medical oncologist and urology oncology surgeon told me about a year after I completed treatment that neither of them thought I would survive my encounter with bladder cancer. They were also both convinced that besides my positive, stubborn attitude, my decision to immediately get my diversion was what most assuredly saved my life.
I am alive because I chose my life over my organs. I am alive because I chose to get an ostomy right out of the bladder cancer gate. Seven years later, I am still alive and still cancer-free. I owe it all to my urostomy – the best decision ever!

Liz Hiles resides in her hometown of Cincinnati, Ohio. She was diagnosed with Stage III-b bladder cancer in August 2016. She had a radical cystectomy with radical hysterectomy and stoma placement for a urostomy in September 2016. She has been sharing her story and advocating for AYA cancer, bladder cancer, and ostomies ever since.
