Community Connection | IBD

This post was brought to you from Tina Aswani-Omprakash of Own Your Crohn’s as part of Girls With Gut’s Community Connection.
My name is Anisha Gangotra, I’m 37 years old and I live in Buckinghamshire in the United Kingdom. I’ve lived with ulcerative colitis since 2008, from the age of 24. I experienced my first colitis symptoms following a two-week holiday abroad. My stomach hadn’t felt quite right but I’d also had my period when I was on holiday so I assumed that it was a mixture of jet lag, my body adjusting to a different environment and my menstrual cycle. I’ve always had a sensitive stomach so I didn’t think much of it. When I returned home, I noticed blood in my poo. I knew then that something wasn’t right and went straight to my family doctor, which kick-started my journey of living with a chronic illness.
Like many ulcerative colitis warriors, my path to diagnosis wasn’t a straightforward process. Over two years, I had many appointments, saw different doctors at different hospitals, had various diagnoses and prognoses thrown about and at one point, the doctor I was seeing thought there was nothing wrong with me and wanted to discharge me from care! The first-ever colonoscopy I had was beyond traumatizing. I was in the midst of a flare-up and wasn’t given any bowel prep or any sedation and they wanted to do a full colonoscopy whilst my bowels were full!
After two years of losing weight, being unable to eat properly, running to the bathroom up to 20 times a day and bleeding, I came under the care of my current gastroenterologist and was finally given an official diagnosis of ulcerative colitis in 2010. It was a relief to know that someone finally believed my symptoms and the impact it was having on my quality of life. The difference between my current gastroenterologist and the other doctors I had seen was that she listened to me, understood and clearly explained what was going on instead of making me think I was crazy and imagining it all. I’ve now spent 10 years traveling 90 miles for appointments to remain under the care of this gastroenterologist because we have a relationship of mutual trust, respect and shared decision-making in my care.
I’ve been on many medications over the years and it’s been a challenge to find what works for me and would keep me in remission. I’ve been on steroids, used enemas and suppositories, tried mesalamines, immuno-modulators and in recent years, I went on to try biologics. It took 10 years to find a medication that would induce remission. It’s been a tiring, frustrating journey. Nevertheless, I’m hopeful for the future. There’s been so much progress since I’ve been diagnosed and there are so many more medications available now to patients.
As if living with colitis wasn’t challenging enough, in 2011, I was the victim of a non-fault, high speed car accident along a dual carriageway. I can still see it clearly in my mind, like something out of an action movie – flying cars and crushing metal. The emergency services couldn’t believe I’d survived the crash. I had physical injuries and suffered with Post-Traumatic Stress Disorder (PTSD), depression and anxiety for the following 5 years. I’d spent three years coming to terms with the physical and mental health challenges of living with colitis. At this point, I was facing yet another challenge. My colitis wasn’t well-controlled and I was managing constant flares alongside the chronic pain and mental health issues from the accident. I was in the midst of some truly dark times.
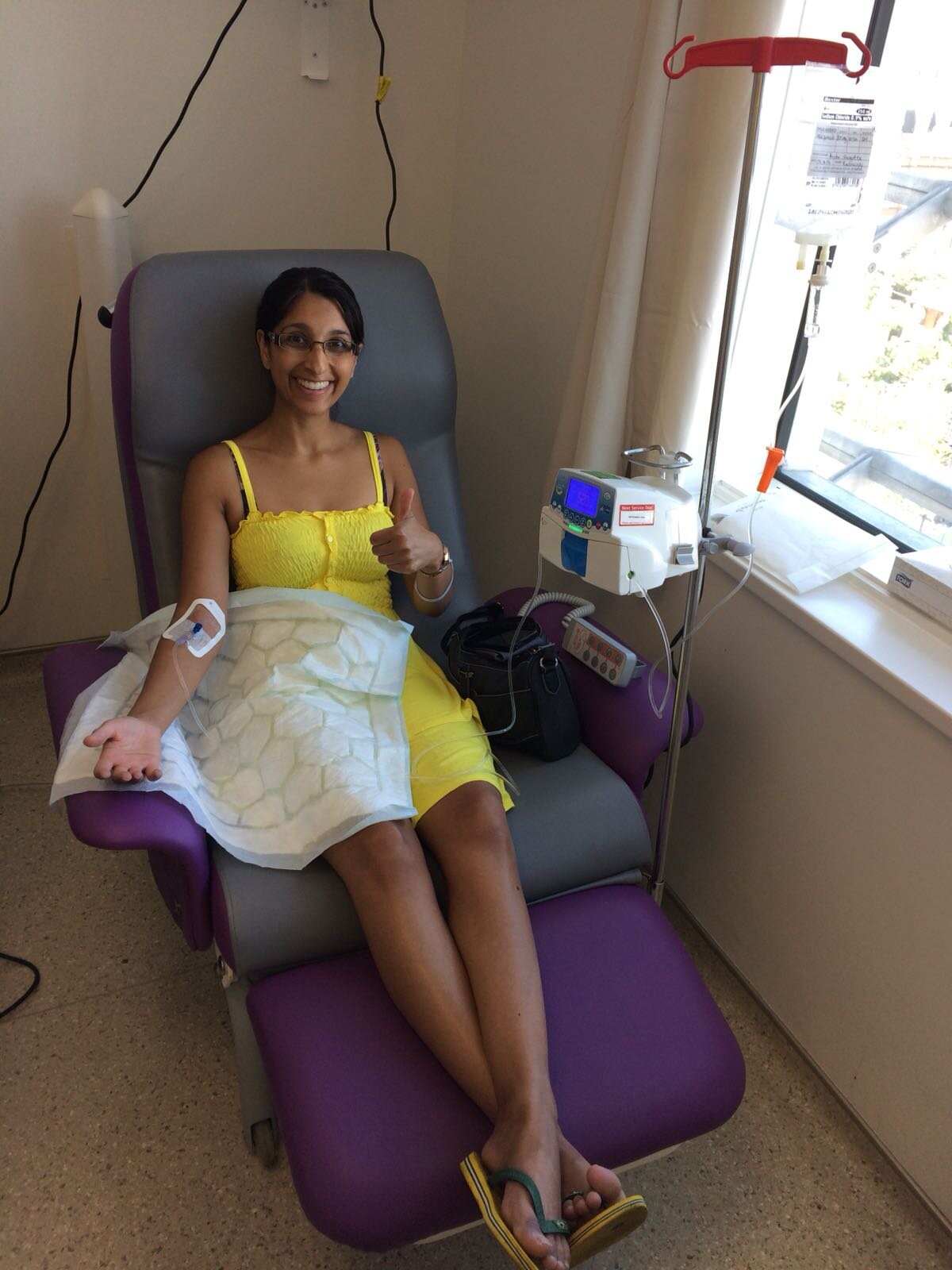
These two life-changing events affected everything – home life, work, friendships, relationships, socializing and hobbies. I had been playing field hockey from a very young age and it was my main form of exercise and stress relief. I’d found it increasingly difficult to continue playing as my colitis wasn’t well managed. So I decided to return to dancing, which I had done intermittently over the years. It felt a bit more manageable and less competitive than field hockey. As soon as I started to get back into dancing, that was when the car accident happened.
So what was I supposed to do now? I could barely get out of bed by myself, had constant pain and a limited range of movement. As I worked through my rehab over months and years, literally step by step, I decided to try a Zumba class. And I’ve never looked back since. I did what I could based on my injuries and slowly regained strength and flexibility. I was struggling with the PTSD, depression and anxiety but by attending classes, I found myself becoming a part of a community – a community that loved to dance their cares away. It was exactly what I needed.
I have always loved traveling and I took the plunge to go to South America alone and do a mixture of traveling and voluntary work. It was a challenge traveling with sometimes patchy toilet facilities and long bus journeys as well as carrying 5 months worth of medication. Nevertheless, it was one of the most courageous decisions I ever made to date. I went to Carnival in Brazil, a traditional gaucho festival in Argentina, The Salt Flats in Bolivia and whilst I was in Chile, I connected with the Chilean Crohn’s and Colitis group. I even went on a march in support of changes needed in the Chilean health and welfare system to support people with chronic health conditions. There was a festival-like atmosphere with music and entertainment but the importance of the march was not lost; it really brought home that no matter where you’re from or what condition you have, being just one more voice can lend weight to a cause.

My life’s path completely changed. I became a licensed Zumba instructor in 2014 and subsequently gained an Inclusive Dance qualification with ParaDance UK. I wanted to provide a safe space for all, including those with disabilities, long-term conditions and mental health issues to enjoy the physical and mental benefits of dance. I have students with cerebral palsy, multiple sclerosis, lung conditions, depression and amputees, all dancing alongside those with no physical or mental health conditions. Everyone does what they feel comfortable. There’s no pressure or judgement. We dance, sweat and, most importantly, have fun! It’s allowed me to stay active in a manageable way, particularly as fatigue is one of my most difficult colitis symptoms to manage. I’ve also used dance to bring people together, increase awareness and raise funds for various causes. I’ve done themed classes to support Crohn’s and Colitis UK, inclusive dance warm-ups at big fundraisers and dance videos for charities like the MS Society, Sue Ryder and MS Trust. As the pandemic took over in early 2020, I have since been teaching online since the Covid-19 pandemic. It has provided a space to have an open dialogue about the issues we’re facing while sharing our personal challenges. That in itself, has been truly powerful.
I’ve had various forms of psychological therapy over the years. I had done some Cognitive Behavioral Therapy (CBT) for IBS in the early years whilst the doctors were still trying to reach a diagnosis but other than that, I’d never really had much support with my mental health and colitis. I was mostly always asked about my physical symptoms but not how I was coping mentally. It was when I started to experience extreme fatigue in 2016 that I was offered a course for people living with long-term conditions which covered aspects such as sleep hygiene, pain management and acceptance therapy. Whilst there were aspects of this which were helpful, it wasn’t specifically tailored to people with IBD. I also had CBT and Eye Movement Desensitization and Reprocessing (EMDR) for the PTSD, depression and anxiety that I experienced from the car accident. The combination of all these therapies has supported my mental health recovery over the years.
As a result of my experiences, I changed careers. I used to work in business for consumer goods companies. For the past 2.5 years now, I’ve been working in the Mental Health Service, specializing in mental health and employment. It’s a truly rewarding job and I give credit to my personal challenges which led me to where I am today.
There’s definitely still a stigma in wider society attached to having a chronic illness or mental health issues. As a woman of South Asian descent, there’s particular stigma in the South Asian communities which can make it even more challenging. Myself and my family – mum, dad and my two sisters – have been open with each other about discussing health issues and we’ve always been supportive of one another but outside of the family in the community, we’ve experienced stigma and ignorance. I’ve heard people say that living with a chronic illness or disability means ‘you’ve done something bad in a previous life and it’s your karma’, basically implying that your illness is all your fault.

Food is also a central part of South Asian culture. When visiting relative’s houses and they offer you something to eat or drink, it’s rude to say no but how do you explain to them that it’ll make you sick and risk running to and from the bathroom for the duration of the visit? I can’t eat dhal (lentils) or chilies as it triggers my symptoms and when I’ve had to explain dietary requirements, I get funny looks as if to say, ‘but you’re Indian, what’s wrong with you?’
I’ve also felt immense guilt when I’ve had to miss out of events. I remember missing my cousin’s wedding reception because my fatigue was so bad that I couldn’t even get out of bed. I felt like I’d let everyone down but trying to explain your condition when people don’t understand can be really challenging and energy-consuming. But the only way we can change this is by making our voices heard, educating, explaining and trying to change attitudes within the community. I don’t want people to feel sorry for me which is usually the first reaction I get. I certainly don’t feel sorry for myself. What I want is acknowledgement and understanding of the strength and determination it takes for people to live with chronic conditions and mental health issues and how much value they contribute to our society. If I could give one piece of advice to someone facing these challenges, it would be to educate yourself about your conditions, so you can educate others, challenge the stereotypes and advocate for yourself.

I have so much experience to share and I didn’t want others living with chronic illness or mental health issues to feel as alone as I did, to experience stigma and discrimination, to struggle to access the right support and treatment at the right time. That’s how I got into advocacy. I’ve told my story at conferences, on social media, on blogs, the radio and on television, in a bid to reduce stigma and put a face to these conditions. My sister, Trishna Bharadia has lived with multiple sclerosis since 2008 and she is well-known in the advocacy world. She is an inspiration for me and others in this field who want to make a difference. The most important part of being able to share my story has been coming out of the other side of those truly dark times, having acceptance of the struggles I faced and not feeling ashamed of it but empowered by it.
My advocacy work led to my nomination for the 9th Annual WEGO Health Awards in the ‘Rookie of the Year’ category. WEGO Health recognises patient advocates who are leading the way in online health communities across 16 categories and across all conditions, platforms and countries. I was truly honoured to be among the 13,000 nominees across 16 categories from across the globe and to be one of six finalists in this category.
Whilst progress has been made, there is still a way to go. I believe sharing my story and using my experience to work with stakeholders, including healthcare professionals, charities, pharma, patient organizations and the media, we can challenge society’s views of those living with invisible conditions, improve infrastructure to better support us and shape the future of healthcare by the people who use it.
And all the while I can own my ulcerative colitis, own my mental health by dancing my way through it all! I invite you all to join my virtual Zumba classes. Learn more about me on Facebook, Instagram and Twitter: @zumbawithanisha
Anisha Gangotra is a UK-based health advocate and patient leader who has lived with ulcerative colitis since 2008 and mental health issues including PTSD, depression and anxiety following a traumatic, high-speed car accident in 2011. She’s works in the mental health profession specialising in mental health and employment and in her spare time, she’s an Inclusive Dance and Zumba instructor, bringing the joy of dance to people with chronic health conditions, disabilities and mental health issues. She was a finalist in the 9th Annual WEGO Health Awards 2020 which recognises patient advocates who are leading the way in online health communities across the globe. She’s passionate about sharing her story and using her experience to work with multiple stakeholders so we can challenge society’s views of those living with invisible conditions, improve infrastructure to better support us, shape the future of healthcare by the people who use it, and continue to dance whilst doing it!
